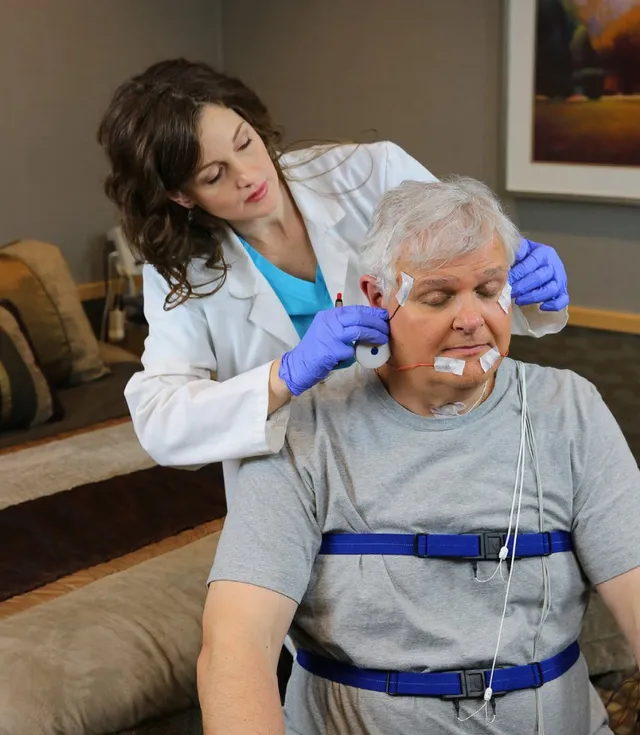
Reliability depends on who is being tested, what type of device is used, and how the results are interpreted by a qualified clinician.
Is a home sleep apnea test in Australia accurate enough to diagnose obstructive sleep apnea?
A sleep apnea home test Australia can be accurate enough to support a diagnosis for people with a high likelihood of moderate to severe obstructive sleep apnea (OSA). Modern home sleep apnea tests typically measure breathing patterns, oxygen levels, heart rate, and airflow, which are key signals for OSA.
However, home tests generally estimate sleep time rather than measuring brain activity, so they can sometimes understate severity, especially if the person is awake for long periods while wearing the device.
What makes lab sleep studies more reliable than home tests?
Lab studies, often called polysomnography, are considered the most comprehensive option because they measure more signals. They can include brain waves (EEG), eye movements, muscle tone, breathing effort, airflow, oxygen saturation, body position, and limb movement.
Because they measure actual sleep stages and total sleep time, labs can produce a more precise apnea-hypopnea index (AHI) and can detect a wider range of sleep disorders beyond OSA.
When is a home sleep apnea test in Australia the right choice?
Home testing is often a strong choice when they have classic OSA symptoms such as loud snoring, witnessed breathing pauses, and significant daytime sleepiness. It can also suit those who are likely to sleep poorly in a lab or who need a faster, more accessible pathway to assessment.
Many Australians choose home tests because they are easier to schedule and can reflect a more typical night’s sleep environment, which can improve comfort and compliance.
Who should avoid home sleep apnea tests and consider lab testing instead?
Home tests may not be appropriate when there is a higher risk of complex sleep-related breathing issues or other conditions that can confuse results. If they have significant heart or lung disease, suspected central sleep apnea, neuromuscular conditions, or persistent symptoms despite a negative home test, lab testing is usually the safer next step.
Lab studies can also be better when there is suspicion of other sleep disorders such as periodic limb movement disorder, narcolepsy, or parasomnias, since home tests generally do not measure the signals needed to detect those.
Can home tests miss mild sleep apnea or underestimate severity?
Yes, home tests can miss mild OSA or underestimate severity in some cases. A common reason is that many home devices calculate breathing events over recording time rather than confirmed sleep time, which can dilute the event rate if they lie awake.
Home tests can also be affected by sensor displacement, poor signal quality, or atypical breathing patterns. That is why clinical context matters, and why a negative home test does not always rule out sleep apnea if symptoms remain strong.
Does the type of home test device affect reliability?
It does. Some home tests use more sensors and offer better signal quality than simpler devices. Reliability improves when the device captures multiple breathing channels and oxygen data clearly throughout the night.
They should also consider whether the test is provided through a medically supervised pathway, since set-up guidance, device quality, and professional interpretation can be the difference between a useful result and an inconclusive one.
How important is clinician interpretation for home sleep apnea test results?
It is critical. A home test report is not just a number; it needs to be interpreted alongside symptoms, medical history, medications, and risk factors. Clinicians can also identify signs of poor data quality and recommend a repeat test or escalation to an in-lab study when needed.

The most reliable outcomes usually come when the home test is part of an end-to-end process that includes screening, appropriate device selection, and follow-up planning. See Medicare coverage for sleep study costs in Australia explained.
What happens if the home test is negative but symptoms continue?
A negative home test should not be treated as the final word if they still have strong symptoms. In that situation, clinicians often recommend either repeating the home test or moving to an in-lab polysomnography, depending on the level of concern and the person’s health profile.
This step matters because untreated sleep apnea can still be present even when a single-night home study fails to capture typical breathing events.
Is home testing better for comfort and real-world sleep quality?
For many people, yes. Sleeping in their own bed can reduce the “first-night effect” that sometimes occurs in labs, where unfamiliar surroundings disrupt sleep. Better comfort can translate into more natural sleep behaviour, which may improve the practical usefulness of the data.
That said, comfort does not automatically guarantee accuracy. A comfortable test still needs clean signals and correct placement to be dependable.
How should they decide between a sleep apnea home test in Australia and lab testing?
They should base the decision on risk level, symptoms, and complexity. Home testing can be a reliable first step when they have straightforward symptoms of OSA and no red flags. Lab testing is usually the better option when their case is complex, when other sleep disorders are suspected, or when previous home testing has been inconclusive.
In practice, many pathways start with home testing and escalate to a lab study only when needed, balancing access, cost, and diagnostic confidence.
FAQs (Frequently Asked Questions)
How accurate is a home sleep apnea test in Australia for diagnosing obstructive sleep apnea?
For individuals with a high likelihood of moderate to severe obstructive sleep apnea (OSA), home sleep apnea tests in Australia can be accurate enough to support a diagnosis. These modern devices typically measure key signals such as breathing patterns, oxygen levels, heart rate, and airflow. However, since they estimate sleep time rather than directly measuring brain activity, they may sometimes understate the severity if the person is awake for extended periods during the test.
What are the advantages of lab sleep studies over home sleep apnea tests?
Lab sleep studies, or polysomnography, are more comprehensive because they measure additional signals including brain waves (EEG), eye movements, muscle tone, breathing effort, oxygen saturation, body position, and limb movement. This allows labs to precisely determine sleep stages and total sleep time, resulting in a more accurate apnea-hypopnea index (AHI) and the ability to detect a wider range of sleep disorders beyond obstructive sleep apnea.
When is a home sleep apnea test the right choice for Australians?
Home testing is often suitable for people exhibiting classic OSA symptoms such as loud snoring, witnessed breathing pauses, and significant daytime sleepiness. It is also ideal for those who may sleep poorly in a lab environment or need quicker and more accessible assessment options. Many Australians prefer home tests because they are easier to schedule and reflect typical sleeping conditions, which can enhance comfort and compliance.

Who should consider lab testing instead of a home sleep apnea test?
Individuals with higher risks of complex sleep-related breathing issues or other health conditions should opt for lab testing. This includes those with significant heart or lung disease, suspected central sleep apnea, neuromuscular disorders, or persistent symptoms despite negative home test results. Lab studies are also preferable when other sleep disorders like periodic limb movement disorder, narcolepsy, or parasomnias are suspected since home tests typically cannot detect these conditions.
Can home sleep apnea tests miss mild cases or underestimate the severity of OSA?
Yes, home tests can sometimes miss mild obstructive sleep apnea or underestimate its severity. Many devices calculate breathing events over total recording time rather than confirmed sleep time, which may dilute event rates if the person is awake during testing. Additionally, factors like sensor displacement, poor signal quality, or atypical breathing patterns can affect accuracy. Therefore, clinical context is essential, and a negative home test does not always rule out OSA if symptoms persist.
How important is clinician interpretation in evaluating home sleep apnea test results?
Clinician interpretation is critical for accurate diagnosis from home sleep apnea tests. Test reports must be analyzed alongside symptoms, medical history, medications, and risk factors. Skilled clinicians can identify poor data quality and recommend repeat testing or escalation to in-lab studies when necessary. The most reliable outcomes occur when home testing is integrated into an end-to-end process involving proper screening, device selection, and follow-up care.